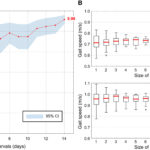
Tracking progression of Parkinson’s disease (PD) requires long visits to the clinic and is subjected to several biases. To facilitate objective evaluation of disease state in individuals with PD, Liu et al. developed a home device able to detect and analyze movements of individuals while performing day-to-day activities. The device emits radio waves and detects them after they bounce back off the people’s body, inferring gait speed. Testing in 50 participants showed that the device performed better than the gold standard in tracking disease progression over time and was able to detect positive response to treatment, suggesting that at-home continuous monitoring could improve disease management in individuals with PD.

There are currently no effective biomarkers for diagnosing Parkinson’s disease (PD) or tracking its progression. Here, we developed an artificial intelligence (AI) model to detect PD and track its progression from nocturnal breathing signals. The model was evaluated on a large dataset comprising 7,671 individuals, using data from several hospitals in the United States, as well as multiple public datasets. The AI model can detect PD with an area-under-the-curve of 0.90 and 0.85 on held-out and external test sets, respectively. The AI model can also estimate PD severity and progression in accordance with the Movement Disorder Society Unified Parkinson’s Disease Rating Scale (R = 0.94, P = 3.6 × 10–25). The AI model uses an attention layer that allows for interpreting its predictions with respect to sleep and electroencephalogram. Moreover, the model can assess PD in the home setting in a touchless manner, by extracting breathing from radio waves that bounce off a person’s body during sleep. Our study demonstrates the feasibility of objective, noninvasive, at-home assessment of PD, and also provides initial evidence that this AI model may be useful for risk assessment before clinical diagnosis.

Insomnia is the most prevalent sleep disorder in the US. In-home insomnia monitoring is important for both diagnosis and treatment. Existing solutions, however, require the user to either maintain a sleep diary or wear a sensor while sleeping. Both can be quite cumbersome. This paper introduces EZ-Sleep, a new approach for monitoring insomnia and sleep.
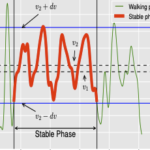
Gait velocity and stride length are critical health indicators for older adults. A decade of medical research shows that they provide a predictor of future falls, hospitalization, and functional decline among seniors. However, currently these metrics are measured only occasionally during medical visits. Such infrequent measurements hamper the opportunity to detect changes and intervene early in the impairment process.

We focus on predicting sleep stages from radio measurements without any attached sensors on subjects. We introduce a new predictive model that combines convolutional and recurrent neural networks to extract sleep-specific subjectinvariant features from RF signals and capture the temporal progression of sleep. A key innovation underlying our approach is a modified adversarial training regime that discards extraneous information specific to individuals or measurement conditions, while retaining all information relevant to the predictive task. We analyze our game theoretic setup and empirically demonstrate that our model achieves significant improvements over state-of-the-art solutions.

RF-Pose provides accurate human pose estimation through walls and occlusions. It leverages the fact that wireless signals in the WiFi frequencies traverse walls and reflect off the human body. It uses a deep neural network approach that parses such radio signals to estimate 2D poses. RF-Pose is trained using state-of-the-art vision model to provide cross-modal supervision. Once trained, RF-Pose uses only the wireless signal for pose estimation. Experimental results show that, when tested on visible scenes, the radio-based system is almost as accurate as the vision-based system used to train it. Yet, unlike vision-based pose estimation, the radio-based system can estimate 2D poses through walls despite never trained on such scenarios.

Understanding users’ behavior at home is central to behavioral research. For example, social researchers are interested in studying domestic abuse, and healthcare professionals are interested in caregiver-patient interaction. Today, such studies rely on diaries and questionnaires, which are subjective, erroneous, and hard to sustain in longitudinal studies

FSHD is a rare, slowly progressive myopathy characterized by weakness initially in facial, shoulder, and upper limb muscles followed by abdominal and paraspinal weakness, and finally lower extremity weakness. FSHD affects between 16,000–38,000 people in the US, and its symptoms often progress over decades, creating significant challenges in tracking disease progression using in-clinic scales and functional tests.


To assess the feasibility of a non-contact radio sensor as an objective measurement tool to study postoperative recovery from endometriosis surgery.

Errors in medication self-administration (MSA) lead to poor treatment adherence, increased hospitalizations and higher healthcare costs. These errors are particularly common when medication delivery involves devices such as inhalers or insulin pens. We present a contactless and unobtrusive artificial intelligence (AI) framework that can detect and monitor MSA errors by analyzing the wireless signals in the patient’s home, without the need for physical contact.